Bone tissue status in women-nuns: age-related features and correlational analysis
DOI:
https://doi.org/10.15587/2519-4798.2026.359662Keywords:
women-nuns, bone tissue, osteopenia, osteoporosis, ultrasound densitometry, age-related changes, correlation analysisAbstract
Bone health is an important indicator of women’s overall well-being, and its age-related decline is often accompanied by the development of osteopenia and osteoporosis. In women living in monastic communities, lifestyle characteristics, dietary patterns, physical activity level, and somatic comorbidities may influence bone remodeling processes, making the assessment of their bone status a relevant task for clinical and preventive medicine.
The aim of research – to assess the bone status of women-nuns using ultrasound densitometry, determine its age-related characteristics, and analyze selected correlation relationships.
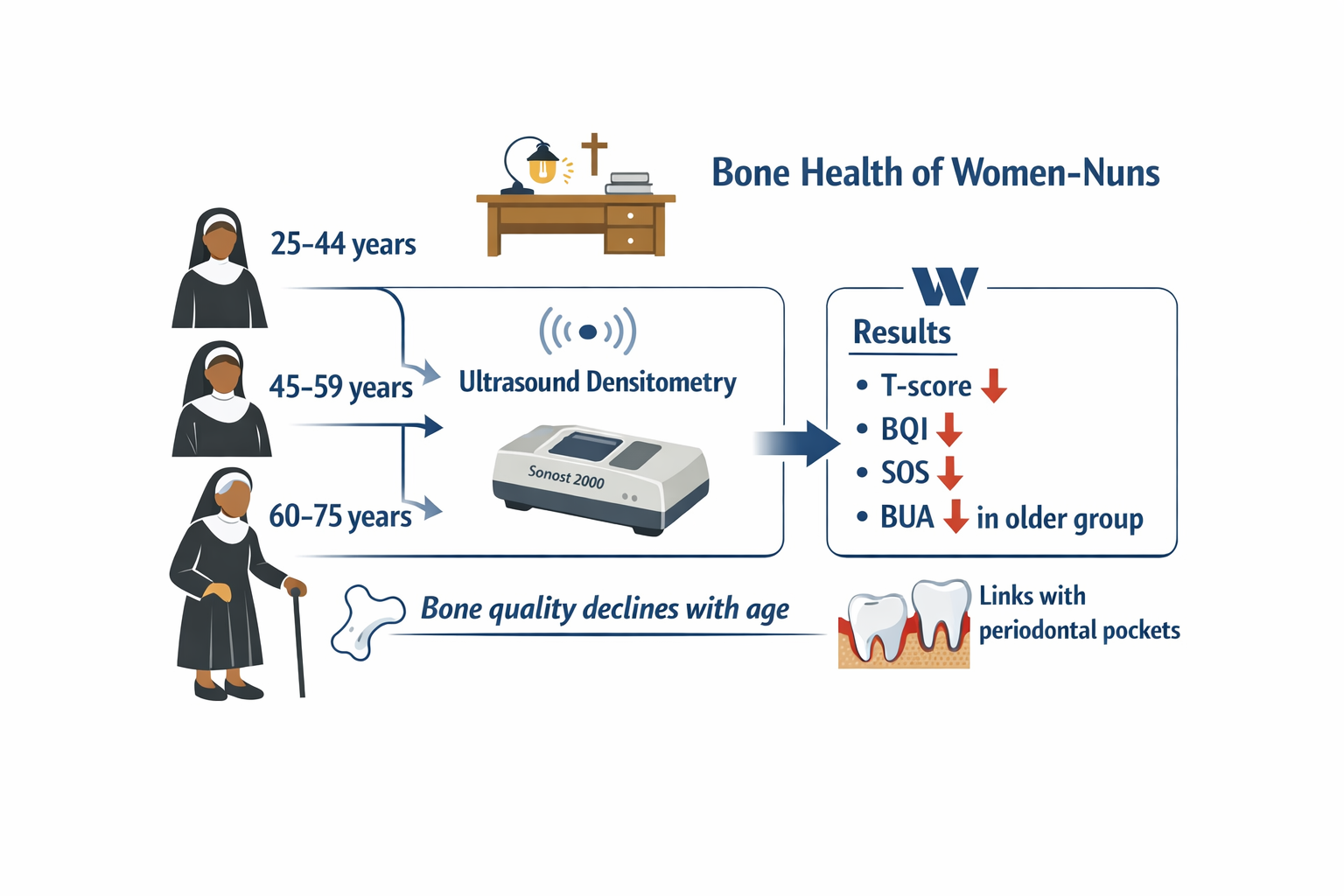
Materials and methods. Twenty-nine women-nuns aged 27–70 years were examined. The participants were divided into age groups according to WHO recommendations: 25–44 years, 45–59 years, and 60–75 years. Bone tissue status was assessed using ultrasound densitometry (Sonost 2000, OsteoSys, Korea). Data on somatic pathology were collected through standardized interviews. Statistical analysis included the Shapiro–Wilk test, the Kruskal–Wallis test, and Pearson correlation; p < 0.05 was considered statistically significant.
Results. Ultrasound densitometry parameters demonstrated a clear age-related decline in bone tissue quality. The 60–75-year group had the lowest T-score values, a pronounced reduction of BQI, and decreased SOS and BUA, reflecting impaired microarchitecture and increased bone fragility. Osteopenia predominated (51.7%), while osteoporosis was identified in 6.9% of participants. The frequency of pathological T-scores increased with age. Correlations between the most common types of somatic pathology and bone tissue parameters were weak and statistically non-significant (r ranging from -0.27 to +0.10). Negative correlations were found between T-score and periodontal pocket depth (r = –0.39; p < 0.05), as well as between SOS and this parameter (r = –0.41; p < 0.05). Other correlations between densitometric and periodontal parameters were statistically non-significant (p > 0.05).
Conclusions. Women-nuns demonstrate a pronounced age-related decline in ultrasound densitometry indices, reflecting reduced mineral density and deterioration of bone quality. Age is the principal determinant of bone status deterioration. The observed negative correlations between bone parameters and selected periodontal indices suggest a possible systemic relationship between structural-functional bone characteristics and the severity of periodontal destruction. These findings emphasize the importance of early detection of bone tissue disorders and comprehensive assessment of oral health among middle-aged and elderly women
References
- Stokes, G., Herath, M., Samad, N., Trinh, A., Milat, F. (2025). ‘Bone Health – Across a Woman’s Lifespan’. Clinical Endocrinology, 102 (4), 389–402. https://doi.org/10.1111/cen.15203
- Osteoporosis management and fracture prevention in postmenopausal women and men over 50 years of age (2024). Healthy Bones Australia. East Melbourne: RACGP. Available at: https://healthybonesaustralia.org.au/wp-content/uploads/2024/03/hba-racgp-guidelines-2024.pdf
- Ahmad, S., Tahir, N., Nauman, R., Gupta, A., Gewelber, C., Batra, K., Izuora, K. (2024). Association between Periodontal Disease and Bone Loss among Ambulatory Postmenopausal Women: A Cross-Sectional Study. Journal of Clinical Medicine, 13 (19), 5812. https://doi.org/10.3390/jcm13195812
- LeBoff, M. S., Greenspan, S. L., Insogna, K. L., Lewiecki, E. M., Saag, K. G., Singer, A. J., Siris, E. S. (2022). The clinician’s guide to prevention and treatment of osteoporosis. Osteoporosis International, 33 (10), 2049–2102. https://doi.org/10.1007/s00198-021-05900-y
- Gregson, C. L., Armstrong, D. J., Bowden, J., Cooper, C., Edwards, J., Gittoes, N. J. L. et al. (2022). UK clinical guideline for the prevention and treatment of osteoporosis. Archives of Osteoporosis, 17 (1). https://doi.org/10.1007/s11657-022-01061-5
- Oheim, R., Tsourdi, E., Seefried, L., Beller, G., Schubach, M., Vettorazzi, E. et al. (2022). Genetic Diagnostics in Routine Osteological Assessment of Adult Low Bone Mass Disorders. The Journal of Clinical Endocrinology & Metabolism, 107 (7), e3048–e3057. https://doi.org/10.1210/clinem/dgac147
- Qi, J., Chen, J., Pang, Y., Guo, Y., Chen, G., Liu, Y., Wang, J., Liu, E. (2023). Association between periodontal disease and osteoporosis in postmenopausal women: A systematic review and meta-analysis. Heliyon, 9 (11), e20922. https://doi.org/10.1016/j.heliyon.2023.e20922
- Elliott, M. E., Martin, B. A., Kanous, N. L., Carnes, M., Komoroske, B., Binkley, N. C. (2003). Risk for Osteoporosis in Elderly Nuns: Need for Better Recognition and Treatment. Current Therapeutic Research, 64 (2), 65–80. https://doi.org/10.1016/s0011-393x(03)00017-1
- Nuzzo, V., Zuccoli, A., de Terlizzi, F., Colao, A., Tauchmanova, L. (2013). Low 25-Hydroxyvitamin D Levels and Low Bone Density Assessed by Quantitative Ultrasonometry in a Cohort of Postmenopausal Italian Nuns. Journal of Clinical Densitometry, 16 (3), 308–312. https://doi.org/10.1016/j.jocd.2012.05.009
- Gani, L. U., Sritara, C., Blank, R. D., Chen, W., Gilmour, J., Dhaliwal, R., Gill, R. (2024). Follow-up Bone Mineral Density Testing: 2023 Official Positions of the International Society for Clinical Densitometry. Journal of Clinical Densitometry, 27 (1), 101440. https://doi.org/10.1016/j.jocd.2023.101440
- Holovanova, I. A., Bielikova, I. V., Liakhova, N. O. (2017). Osnovy medychnoi statystyky. Poltava, 113. Available at: https://repository.pdmu.edu.ua/items/3d7e3785-6ead-44d3-9023-e4aae2b28c0c
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Hanna Babenia, Oksana Dienha, Eduard Dienha

This work is licensed under a Creative Commons Attribution 4.0 International License.
Our journal abides by the Creative Commons Attribution 4.0 International License copyright rights and permissions for open access journals.
Authors, who are published in this journal, agree to the following conditions:
1. The authors reserve the right to authorship of the work and pass the first publication right of this work to the journal under the terms of a Creative Commons Attribution 4.0 International License, which allows others to freely distribute the published research with the obligatory reference to the authors of the original work and the first publication of the work in this journal.
2. The authors have the right to conclude separate supplement agreements that relate to non-exclusive work distribution in the form in which it has been published by the journal (for example, to upload the work to the online storage of the journal or publish it as part of a monograph), provided that the reference to the first publication of the work in this journal is included.
3. Authors have the right to store the final accepted version of the article in an institutional, thematic, or any other repository to ensure visibility and accessibility.







