Analysis of the current state of development of micro-needle systems for transdermal drug delivery (a scoping review)
DOI:
https://doi.org/10.15587/2519-4852.2026.352761Keywords:
microneedle system, transdermal delivery, improved penetration of active substances, bibliosemantic analysisAbstract
The aim is to examine the current state of development of microneedle systems for transdermal drug delivery.
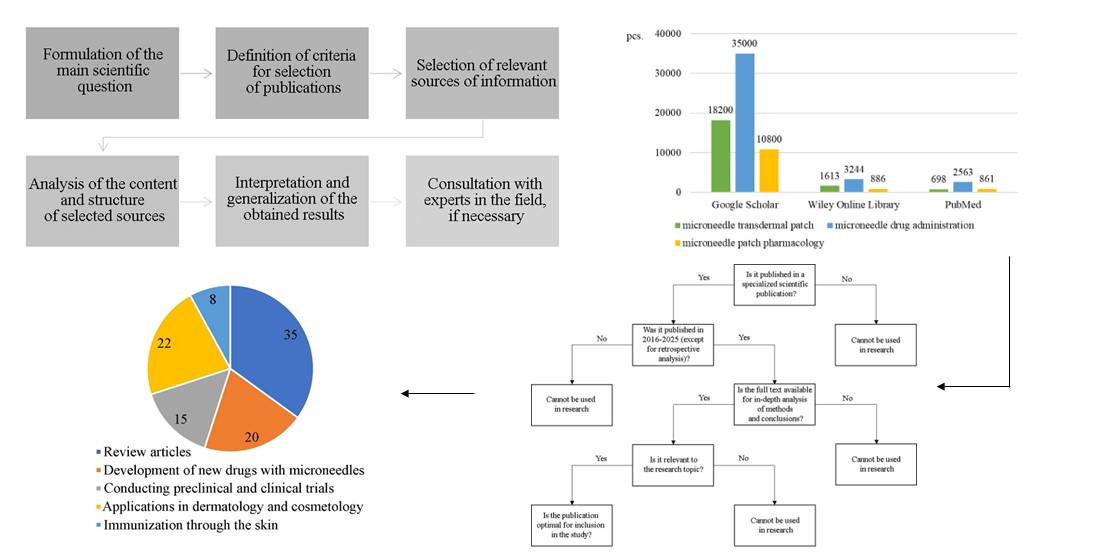
Materials and methods. Analysis, systematization, and generalization of data from scientific literature sources on the development of microneedle systems, research on their effectiveness, and prospects for use in pharmacy. A modified Arskey O'Malley methodology was used, refined by a research group led by H.M. Daudt. A total of 480 publications from the last ten years were analysed.
Results. The results of the analysis show that most of the experimental studies focus on the development of microneedle systems for transdermal delivery of vaccines, insulin, and analgesics. In contrast, studies devoted to the creation of drugs with a different direction of action or drugs for the gradual release of active substances using microneedles occupy a smaller segment of the total number.
Conclusions. It has been established that most scientists choose to develop microneedle-based drugs for systemic use. The main areas of publication are reviews of literature sources, the development of new microneedle systems, etc. The results obtained indicate the potential and relevance of conducting research on the development of microneedle systems
References
- Daudt, H. M., van Mossel, C., Scott, S. J. (2013). Enhancing the scoping study methodology: a large, inter-professional team’s experience with Arksey and O’Malley’s framework. BMC Medical Research Methodology, 13 (1). https://doi.org/10.1186/1471-2288-13-48
- Ledger, P. W., Nichols, K. C. (1989). Transdermal drug delivery devices. Clinics in Dermatology, 7 (3), 25–31. https://doi.org/10.1016/0738-081x(89)90004-7
- Henry, S., McAllister, D. V., Allen, M. G., Prausnitz, M. R. (1998). Microfabricated Microneedles: A Novel Approach to Transdermal Drug Delivery. Journal of Pharmaceutical Sciences, 87 (8), 922–925. https://doi.org/10.1021/js980042+
- Prausnitz, M. R., Langer, R. (2008). Transdermal drug delivery. Nature Biotechnology, 26 (11), 1261–1268. https://doi.org/10.1038/nbt.1504
- Gill, H. S., Prausnitz, M. R. (2007). Coated microneedles for transdermal delivery. Journal of Controlled Release, 117 (2), 227–237. https://doi.org/10.1016/j.jconrel.2006.10.017
- Davis, S. P., Martanto, W., Allen, M. G., Prausnitz, M. R. (2005). Hollow Metal Microneedles for Insulin Delivery to Diabetic Rats. IEEE Transactions on Biomedical Engineering, 52 (5), 909–915. https://doi.org/10.1109/tbme.2005.845240
- Ameri, M., Kadkhodayan, M., Nguyen, J., Bravo, J., Su, R., Chan, K. et al. (2014). Human Growth Hormone Delivery with a Microneedle Transdermal System: Preclinical Formulation, Stability, Delivery and PK of Therapeutically Relevant Doses. Pharmaceutics, 6 (2), 220–234. https://doi.org/10.3390/pharmaceutics6020220
- Kim, Y.-C., Park, J.-H., Prausnitz, M. R. (2012). Microneedles for drug and vaccine delivery. Advanced Drug Delivery Reviews, 64 (14), 1547–1568. https://doi.org/10.1016/j.addr.2012.04.005
- Donnelly, R. F., McCrudden, M. T. C., Zaid Alkilani, A., Larrañeta, E., McAlister, E., Courtenay, A. J. et al. (2014). Hydrogel-Forming Microneedles Prepared from “Super Swelling” Polymers Combined with Lyophilised Wafers for Transdermal Drug Delivery. PLoS ONE, 9 (10), e111547. https://doi.org/10.1371/journal.pone.0111547
- Zhang, Y. S., Yue, K., Aleman, J., Mollazadeh-Moghaddam, K., Bakht, S. M., Yang, J. et al. (2016). 3D Bioprinting for Tissue and Organ Fabrication. Annals of Biomedical Engineering, 45 (1), 148–163. https://doi.org/10.1007/s10439-016-1612-8
- Kulkarni, D., Damiri, F., Rojekar, S., Zehravi, M., Ramproshad, S., Dhoke, D. et al. (2022). Recent Advancements in Microneedle Technology for Multifaceted Biomedical Applications. Pharmaceutics, 14 (5), 1097. https://doi.org/10.3390/pharmaceutics14051097
- Gowda, B. H. J., Ahmed, M. G., Sahebkar, A., Riadi, Y., Shukla, R., Kesharwani, P. (2022). Stimuli-Responsive Microneedles as a Transdermal Drug Delivery System: A Demand-Supply Strategy. Biomacromolecules, 23 (4), 1519–1544. https://doi.org/10.1021/acs.biomac.1c01691
- Zulcaif, Zafar, N., Mahmood, A., Sarfraz, R. M., Elaissari, A. (2022). Simvastatin Loaded Dissolvable Microneedle Patches with Improved Pharmacokinetic Performance. Micromachines, 13 (8), 1304. https://doi.org/10.3390/mi13081304
- Sekar, L., Seenivasan, R., Reddy, M. V., Varma, K. D., Ahmed, S. S., Pachiyappan, J. K., Ganesh, G. (2024). Advancements in microneedle technology: comprehensive insights into versatile drug delivery mechanisms. International Journal of Applied Pharmaceutics, 16 (2), 1–11. https://doi.org/10.22159/ijap.2024v16i2.49564
- Zhang, X., Wang, Y., Chi, J., Zhao, Y. (2020). Smart Microneedles for Therapy and Diagnosis. Research, 2020. https://doi.org/10.34133/2020/7462915
- Balde, A., Kim, S.-K., Nazeer, R. A. (2025). A review on microneedle patch as a delivery system for proteins/peptides and their applications in transdermal inflammation suppression. International Journal of Biological Macromolecules, 307, 141963. https://doi.org/10.1016/j.ijbiomac.2025.141963
- Khalid, R., Mahmood, S., Mohamed Sofian, Z., Hilles, A. R., Hashim, N. M., Ge, Y. (2023). Microneedles and Their Application in Transdermal Delivery of Antihypertensive Drugs – A Review. Pharmaceutics, 15 (8), 2029. https://doi.org/10.3390/pharmaceutics15082029
- Gowda, B. H. J., Ahmed, M. G., Thakur, R. R. S., Donnelly, R. F., Vora, L. K. (2024). Microneedles as an Emerging Platform for Transdermal Delivery of Phytochemicals. Molecular Pharmaceutics, 21 (12), 6007–6033. https://doi.org/10.1021/acs.molpharmaceut.4c00894
- Wu, C., Yu, Q., Huang, C., Li, F., Zhang, L., Zhu, D. (2024). Microneedles as transdermal drug delivery system for enhancing skin disease treatment. Acta Pharmaceutica Sinica B, 14 (12), 5161–5180. https://doi.org/10.1016/j.apsb.2024.08.013
- Shin, J. Y., Han, D., Yoon, K. Y., Jeong, D. H., Park, Y. I. (2024). Clinical Safety and Efficacy Evaluation of a Dissolving Microneedle Patch Having Dual Anti-Wrinkle Effects With Safe and Long-Term Activities. Annals of Dermatology, 36 (4), 215–224. https://doi.org/10.5021/ad.23.136
- Chen, J., Ren, H., Zhou, P., Zheng, S., Du, B., Liu, X., Xiao, F. (2022). Microneedle-mediated drug delivery for cutaneous diseases. Frontiers in Bioengineering and Biotechnology, 10. https://doi.org/10.3389/fbioe.2022.1032041
- Jaiswal, S., Jawade, S. (2024). Microneedling in Dermatology: A Comprehensive Review of Applications, Techniques, and Outcomes. Cureus, 16 (9). https://doi.org/10.7759/cureus.70033
- Mashi, A., Oraybi, R. A., Hakami, M. S., Altalhi, A. M., Alrezqi, W. A., Hakami, T. K. et al. (2025). Microneedling for Non-cosmetic Dermatologic Conditions: A Systematic Review of Efficacy and Safety. Cureus, 18 (7). https://doi.org/10.7759/cureus.90857
- Tehrani, L., Tashjian, M., Mayrovitz, H. N. (2025). Physiological Mechanisms and Therapeutic Applications of Microneedling: A Narrative Review. Cureus, 17 (3). https://doi.org/10.7759/cureus.80510
- Vyshnevska, L. I. (2023). Rozchynni mikroholky yak odna z innovatsiinykh tekhnolohii transdermalnykh system dostavky likarskykh preparativ. Suchasni dosiahnennia farmatsevtychnoi spravy. Kharkiv, 138–142. Available at: https://dspace.nuph.edu.ua/bitstream/123456789/30828/1/138-142.pdf
- Wadte, S. S., Hatwar, P. R., Bakal, R. L., Korde, D. V. (2025). Microneedle technology: An innovative approach for transdermal drug delivery and vaccine administration. International Journal of Pharmacy and Pharmaceutical Science, 7 (1), 194–202. https://doi.org/10.33545/26647222.2025.v7.i1c.168
- Zhu, D. D., Zhang, X. P., Zhang, B. L., Hao, Y. Y., Guo, X. D. (2020). Safety Assessment of Microneedle Technology for Transdermal Drug Delivery: A Review. Advanced Therapeutics, 3 (8). https://doi.org/10.1002/adtp.202000033
- Sivamani, R. K., Stoeber, B., Wu, G. C., Zhai, H., Liepmann, D., Maibach, H. (2005). Clinical microneedle injection of methyl nicotinate: stratum corneum penetration. Skin Research and Technology, 11 (2), 152–156. https://doi.org/10.1111/j.1600-0846.2005.00107.x
- Lee, I.-C., He, J.-S., Tsai, M.-T., Lin, K.-C. (2015). Fabrication of a novel partially dissolving polymer microneedle patch for transdermal drug delivery. Journal of Materials Chemistry B, 3 (2), 276–285. https://doi.org/10.1039/c4tb01555j
- Yamagishi, R., Miura, S., Yabu, K., Ando, M., Hachikubo, Y., Yokoyama, Y. et al. (2024). Fabrication Technology of Self-Dissolving Sodium Hyaluronate Gels Ultrafine Microneedles for Medical Applications with UV-Curing Gas-Permeable Mold. Gels, 10 (1), 65. https://doi.org/10.3390/gels10010065
- Zhang, L., Guo, R., Wang, S., Yang, X., Ling, G., Zhang, P. (2021). Fabrication, evaluation and applications of dissolving microneedles. International Journal of Pharmaceutics, 604, 120749. https://doi.org/10.1016/j.ijpharm.2021.120749
- Andranilla, Rr. K., Anjani, Q. K., Hartrianti, P., Donnelly, R. F., Ramadon, D. (2023). Fabrication of dissolving microneedles for transdermal delivery of protein and peptide drugs: polymer materials and solvent casting micromoulding method. Pharmaceutical Development and Technology, 28 (10), 1016–1031. https://doi.org/10.1080/10837450.2023.2285498
- Bai, C., Huo, C., Zhang, P. (2020). Dissolving Microneedles for Transdermal Drug Delivery System. Journal of Physics: Conference Series, 1626 (1), 012104. https://doi.org/10.1088/1742-6596/1626/1/012104
- Yu, X., Zhao, J., Fan, D. (2023). The Progress in the Application of Dissolving Microneedles in Biomedicine. Polymers, 15 (20), 4059. https://doi.org/10.3390/polym15204059
- Yadav, P. R., Hingonia, P., Das, D. B., Pattanayek, S. K. (2024). Modeling of Dissolving Microneedle-Based Transdermal Drug Delivery: Effects of Dynamics of Polymers in Solution. Molecular Pharmaceutics, 21 (10), 5104–5114. https://doi.org/10.1021/acs.molpharmaceut.4c00492
- Bandral, M. R., Padgavankar, P. H., Japatti, S. R., Gir, P. J., Siddegowda, C. Y., Gir, R. J. (2018). Clinical Evaluation of Microneedling Therapy in the Management of Facial Scar: A Prospective Randomized Study. Journal of Maxillofacial and Oral Surgery, 18 (4), 572–578. https://doi.org/10.1007/s12663-018-1155-7
- Hirobe, S., Azukizawa, H., Matsuo, K., Zhai, Y., Quan, Y.-S., Kamiyama, F. et al. (2013). Development and Clinical Study of a Self-Dissolving Microneedle Patch for Transcutaneous Immunization Device. Pharmaceutical Research, 30 (10), 2664–2674. https://doi.org/10.1007/s11095-013-1092-6
- Bahadur, S., Radhika, Sahu, K. K., Singh, A. K. (2025). Advances and Challenges of Microneedle Assisted Drug Delivery for Biomedicals Applications: A Review. Current Pharmaceutical Biotechnology, 26 (16), 2566–2577. https://doi.org/10.2174/0113892010310769240924053724
- Vergilio, M. M., Birchall, J. C., Lima, L. L., Rezende, R. A., Leonardi, G. R. (2024). Drug Delivery Systems based on Microneedles for Dermatological Diseases and Aesthetic Enhancement. Current Medicinal Chemistry, 31 (23), 3473–3487. https://doi.org/10.2174/0929867330666230525122913
- Nagod, S., Halse, D. S. V. (2020). MEMS Based Microneedles in the Field of Drug Delivery. International Journal of Innovative Technology and Exploring Engineering, 9 (4), 2863–2867. https://doi.org/10.35940/ijitee.d1761.029420
- Huang, Y., Yu, H., Wang, L., Shen, D., Ni, Z., Ren, S. et al. (2022). Research progress on cosmetic microneedle systems: Preparation, property and application. European Polymer Journal, 163, 110942. https://doi.org/10.1016/j.eurpolymj.2021.110942
- Huo, T., Zhou, L., Bian, X., Wen, Y. (2025). Advancing microneedle technology for multiple distinct target organs drug delivery through 3D printing: a comprehensive review. Advanced Composites and Hybrid Materials, 8 (3). https://doi.org/10.1007/s42114-025-01336-8
- Lv, X., Xiang, C., Zheng, Y., Zhou, W.-X., Lv, X.-L. (2024). Recent Developments in Using Microneedle Patch Technology as a More Efficient Drug Delivery System for Treating Skin Photoaging. Clinical, Cosmetic and Investigational Dermatology, 17, 2417–2426. https://doi.org/10.2147/ccid.s492774
- Lee, J. Y., Dong, S. H., Ng, K. W., Goh, C. F. (2025). Assessing the integrity and mechanical properties of commercial microneedles: innovation or fad? Drug Delivery and Translational Research, 15 (11), 3986–4003. https://doi.org/10.1007/s13346-025-01888-8
- Shu, W., Lijnse, T., McCartney, F., Brayden, D. J., Ní Annaidh, A., O’Cearbhaill, E. D. (2025). Computational and Experimental Analysis of Drug‐Coated Microneedle Skin Insertion: The Mode of Administration Matters. Advanced Materials Interfaces, 12 (17). https://doi.org/10.1002/admi.202500202
- AL-shaibani, A., Ghareeb, M. M. (2025). Fabrication and Ex-vivo Evaluation of Olanzapine Nanoparticles Based Dissolved Microneedle for Transdermal Delivery. Iraqi Journal of Pharmaceutical Sciences, 34 (2), 155–167. https://doi.org/10.31351/vol34iss2pp155-167
- Sikandar, M., Shoaib, M. H., Yousuf, R. I., Ahmed, F. R., Siddiqui, F., Saleem, M. T., Irshad, A. (2025). Dissolving microneedle patches for transdermal delivery of paroxetine: in-vitro, ex-vivo studies and its PBPK modeling. Therapeutic Delivery, 16 (9), 835–851. https://doi.org/10.1080/20415990.2025.2542721
- Harris, E. (2024). Microneedle Vaccine Patches Generated Immune Response in Children. JAMA, 331 (23), 1982. https://doi.org/10.1001/jama.2024.8629
- Leone, M., Mönkäre, J., Bouwstra, J. A., Kersten, G. (2017). Dissolving Microneedle Patches for Dermal Vaccination. Pharmaceutical Research, 34 (11), 2223–2240. https://doi.org/10.1007/s11095-017-2223-2
- Bhatnagar, S., Chawla, S. R., Kulkarni, O. P., Venuganti, V. V. K. (2017). Zein Microneedles for Transcutaneous Vaccine Delivery: Fabrication, Characterization, and in Vivo Evaluation Using Ovalbumin as the Model Antigen. ACS Omega, 2 (4), 1321–1332. https://doi.org/10.1021/acsomega.7b00343
- Yu, Y., Wang, J., Wu, M. X. (2023). Microneedle-Mediated Immunization Promotes Lung CD8+ T-Cell Immunity. Journal of Investigative Dermatology, 143 (10), 1983-1992.e3. https://doi.org/10.1016/j.jid.2023.03.1672
- Marshall, S., Sahm, L. J., Moore, A. C. (2016). The success of microneedle-mediated vaccine delivery into skin. Human Vaccines & Immunotherapeutics, 12 (11), 2975–2983. https://doi.org/10.1080/21645515.2016.1171440
- Ruan, S., Zhang, Y., Feng, N. (2021). Microneedle-mediated transdermal nanodelivery systems: a review. Biomaterials Science, 9 (24), 8065–8089. https://doi.org/10.1039/d1bm01249e
- Hulimane Shivaswamy, R., Binulal, P., Benoy, A., Lakshmiramanan, K., Bhaskar, N., Pandya, H. J. (2025). Microneedles as a Promising Technology for Disease Monitoring and Drug Delivery: A Review. ACS Materials Au, 5 (1), 115–140. https://doi.org/10.1021/acsmaterialsau.4c00125
- Wang, Z., Xiao, M., Li, Z., Wang, X., Li, F., Yang, H., Chen, Y., Zhu, Z. (2024). Microneedle Patches‐Integrated Transdermal Bioelectronics for Minimally Invasive Disease Theranostics. Advanced Healthcare Materials, 13 (17). https://doi.org/10.1002/adhm.202303921
- Jiang, X., Zeng, Y., Zhang, W., Wang, C., Li, W. (2023). Advances in microneedle patches for long-acting contraception. Acta Materia Medica, 2 (1). https://doi.org/10.15212/amm-2022-0042
- Arshad, M. S., Nazari, K., Rana, S. J., Zafar, S., Uzair, M., Ahmad, Z. (2023). Dissolving Microneedle Patches as Vaccine Delivery Platforms. British Journal of Pharmacy, 8(2). https://doi.org/10.5920/bjpharm.1334
- Shah, S. W. A., Li, X., Yuan, H., Shen, H., Pan, G., Xie, H., Shao, J. (2025). State‐of‐the‐Art Fabrication of Microneedle Patches: A Mini‐Review on Emerging Techniques. MedComm – Biomaterials and Applications, 4 (3). https://doi.org/10.1002/mba2.70020
- Pundir, G., Morris, S., Jakhmola, V., Parashar, T. P. (2024). Microneedle Transdermal Patches- A Novel Painless Approach with Improved Bioavailability for the Treatment of Diseases with Special Prevalence to Neonatal Infection. International Journal of Drug Delivery Technology, 14 (3), 1749–1757. https://doi.org/10.25258/ijddt.14.3.71
- Li, J., Zeng, M., Shan, H., Tong, C. (2017). Microneedle Patches as Drug and Vaccine Delivery Platform. Current Medicinal Chemistry, 24 (22). https://doi.org/10.2174/0929867324666170526124053
- Chauhan, S. S., Lobo, V. M., Borate, S. N., Jagade, S. S., Venuganti, V. V. K. (2022). Microneedle Array Patches for the Delivery of Therapeutic Agents. Smart Nanomaterials in Biomedical Applications. Cham: Springer, 223–267. https://doi.org/10.1007/978-3-030-84262-8_9
- Arangannan, S. (2025). Microneedle patches based on herbal formulations for biofilm disruption and management: a comprehensive review. TMP Universal Journal of Advances in Pharmaceutical Sciences, 1 (2). https://doi.org/10.69557/ac68y940
- Freundlich, E., Shimony, N., Gross, A., Mizrahi, B. (2023). Bioadhesive microneedle patches for tissue sealing. Bioengineering & Translational Medicine, 9 (3). https://doi.org/10.1002/btm2.10578
- Rabiee, N. (2025). Revolutionizing biosensing with wearable microneedle patches: innovations and applications. Journal of Materials Chemistry B, 13 (18), 5264–5289. https://doi.org/10.1039/d5tb00251f
- Yan, Y. (2025). Research progress of artificial intelligence-enabled microneedle technology in the treatment of myocardial infarction. Proceedings of the 4th International Conference on Biomedical and Intelligent Systems. New York: Association for Computing Machinery, 553–558. https://doi.org/10.1145/3745034.3745118
- Patil, G., Patil, C., Patil, H., Nikume, D., Kalal, A. (2025). A review on microneedle patches transdermal drug delivery system. International Journal of Advanced Research in Science, Communication and Technology, 5 (2), 382–397. https://doi.org/10.48175/ijarsct-23045
- Zhang, C. Y., Zhang, X., Zhao, X., Li, Y., Zhang, W., Chen, Y. et al. (2025). Dissolved Bubble Microneedle Patches for Co-Delivery of Hydrophobic and Hydrophilic Drugs to Improve Acne Vulgaris Therapy. https://doi.org/10.21203/rs.3.rs-7269052/v1
- Seema, M., Veeresh, T., Muthukumar, S. P. (2025). Boosting Curcumin Bioavailability: Unveiling the Potential of Sodium Caseinate Nanoparticle Microneedle Patches. Polymers for Advanced Technologies, 36 (8). https://doi.org/10.1002/pat.70279
- Lammerding, L. C., Breitkreutz, J. (2023). Technical evaluation of precisely manufacturing customized microneedle array patches via inkjet drug printing. International Journal of Pharmaceutics, 642, 123173. https://doi.org/10.1016/j.ijpharm.2023.123173
- Fahad, F., Ahn, M., Soo Kim, B. (2025). Advanced 3D-printed microneedle patches for smart drug delivery in wound care. International Journal of Bioprinting, 8514. https://doi.org/10.36922/ijb.8514
- Zhang, S., Wei, M., Luan, C., Gao, B. (2025). Bioinspired wearable polymer microneedle patches: pioneering diabetic wound therapy for the horizon. RSC Advances, 15 (39), 32509–32535. https://doi.org/10.1039/d5ra02557e
- Tabriz, A. G., Viegas, B., Okereke, M., Uddin, M. J., Lopez, E. A., Zand, N. et al. (2022). Evaluation of 3D Printability and Biocompatibility of Microfluidic Resin for Fabrication of Solid Microneedles. Micromachines, 13 (9), 1368. https://doi.org/10.3390/mi13091368
- Rajabi, M., Roxhed, N., Shafagh, R. Z., Haraldson, T., Fischer, A. C., Wijngaart, W. van der et al. (2016). Flexible and Stretchable Microneedle Patches with Integrated Rigid Stainless Steel Microneedles for Transdermal Biointerfacing. PLOS ONE, 11 (12), e0166330. https://doi.org/10.1371/journal.pone.0166330
- Su, Y., Shahriar, S. S. M., Andrabi, S. M., Wang, C., Sharma, N. S., Xiao, Y. et al. (2024). It Takes Two to Tangle: Microneedle Patches Co‐delivering Monoclonal Antibodies and Engineered Antimicrobial Peptides Effectively Eradicate Wound Biofilms. Macromolecular Bioscience, 24 (5). https://doi.org/10.1002/mabi.202300519
- Lin, X., Jia, Q., Lin, X., Shi, J., Gong, W., Shen, K. et al. (2025). Galvanic Cell Bipolar Microneedle Patches for Reversing Photoaging Wrinkles. Advanced Materials, 37 (16). https://doi.org/10.1002/adma.202500552
- Sun, L., Fan, L., Bian, F., Chen, G., Wang, Y., Zhao, Y. (2021). MXene-Integrated Microneedle Patches with Innate Molecule Encapsulation for Wound Healing. Research, 2021. https://doi.org/10.34133/2021/9838490
- Nadeem, A. Y., Ul Islam, M., Khan, S., Al-Suhaimi, E. A., Shehzad, A., Noor, A. (2025). Transdermal glucose responsive composite polymeric microneedle patches for personalized diabetes treatment: A novel approach to precision medicine. Journal of Drug Delivery Science and Technology, 111, 107161. https://doi.org/10.1016/j.jddst.2025.107161
- Arshad, M. S., Gulfam, S., Zafar, S., Jalil, N. A., Ahmad, N., Qutachi, O. et al. (2022). Engineering of tetanus toxoid-loaded polymeric microneedle patches. Drug Delivery and Translational Research, 13 (3), 852–861. https://doi.org/10.1007/s13346-022-01249-9
- Coates, I. A., Driskill, M. M., Rajesh, N. U., Lipkowitz, G., Ilyin, D., Xu, Y. et al. (2025). Free-Form Microfluidic Microneedle Array Patches. https://doi.org/10.1101/2025.02.03.635973
- Zeng, J., Lu, M., Wang, Y., Zhao, X., Zhao, Y. (2024). Photothermal Fish Gelatin‐Graphene Microneedle Patches for Chronic Wound Treatment. Small, 20 (48). https://doi.org/10.1002/smll.202405847
- Fan, L., Wang, Y., Wang, L., Lin, X., Wang, X., Shang, L. et al. (2025). Breathable core–shell microneedle patches for diabetic wound treatment. Materials Futures, 4 (2), 025402. https://doi.org/10.1088/2752-5724/adcbc6
- González García, L. E., MacGregor, M., Cavallaro, A., Koynov, K., Vasilev, K. (2022). Plasma polymer barrier layers to control the release kinetics from dissolvable microneedle patches. Plasma Processes and Polymers, 19 (12). https://doi.org/10.1002/ppap.202200099
- Jeong, J.-O., Lim, Y.-M., Lee, J. Y., Park, J.-S. (2023). Polyvinylpyrrolidone based graphene oxide hydrogels by radiation crosslinking for conductive microneedle patches. European Polymer Journal, 184, 111726. https://doi.org/10.1016/j.eurpolymj.2022.111726
- Gan, J., Sun, L., Tang, W., Zhao, Y., Bi, Y. (2025). Separable cryo-microneedle patches delivery with capsaicin integrated mesoporous dopamine for obesity treatment. Journal of Nanobiotechnology, 23 (1). https://doi.org/10.1186/s12951-025-03645-y
- Roy, S., Ghosh, B., Chandra, A., Das, D., Ghosh, P., Choudhury, S., Bose, A., Dinda, S. C. (2025). Enhanced bioavailability of lobeglitazone via dissolving microneedle patches in rats. International Journal of Applied Pharmaceutics, 17, 488–498. https://doi.org/10.22159/ijap.2025v17i5.54818
- Balghonaim, F. A., Chandru, K. K., Krishnegowda, M. B., Naveen, N. R., Goudanavar, P., Joshi, V. et al. (2025). Formulation and Evaluation of Bosentan Monohydrate-loaded Liposome-based Dissolving Microneedle Array Patches. Journal of Pharmacology and Pharmacotherapeutics, 17 (1), 37–52. https://doi.org/10.1177/0976500x251327444
- Arshad, M. S., Zafar, S., Zahra, A. T., Zaman, M. H., Akhtar, A., Kucuk, I. et al. (2020). Fabrication and characterisation of self-applicating heparin sodium microneedle patches. Journal of Drug Targeting, 29 (1), 60–68. https://doi.org/10.1080/1061186x.2020.1795180
- Fan, L., Wang, L., Wang, X., Li, M., Gu, H., Zhang, H. (2025). Multifunctional Silk and Gelatin Composed Microneedle Patches for Enhanced Wound Healing. Smart Medicine, 4 (1). https://doi.org/10.1002/smmd.137
- Su, Y., Andrabi, S. M., Shahriar, S. M. S., Wong, S. L., Wang, G., Xie, J. (2023). Triggered release of antimicrobial peptide from microneedle patches for treatment of wound biofilms. Journal of Controlled Release, 356, 131–141. https://doi.org/10.1016/j.jconrel.2023.02.030
- Ali, S., Ahmad, Z., Mahmood, A., Khan, M. I., Siddique, W., Latif, R. et al. (2025). Enhanced Transdermal Drug Delivery of Labetalol via Nanoparticle-Loaded Dissolvable Microneedle Patches. BioNanoScience, 15 (1). https://doi.org/10.1007/s12668-025-01799-5
- Hu, F., Gao, Q., Liu, J., Chen, W., Zheng, C., Bai, Q. et al. (2023). Smart microneedle patches for wound healing and management. Journal of Materials Chemistry B, 11 (13), 2830–2851. https://doi.org/10.1039/d2tb02596e
- Wang, X., Zhang, X., Zhao, Y., Zhan, X., Hu, C., Li, H. et al. (2025). Recombinant human collagen microneedle patches loaded with PRP for diabetic wound treatment. Journal of Materials Chemistry B, 13 (31), 9607–9624. https://doi.org/10.1039/d5tb00836k
- Avcil, M., Klokkers, J., Jeong, D., Celik, A. (2025). Efficacy of Dissolvable Microneedle Patches with Skincare Actives in Acne Management: A Monocentric Clinical Study. Biologics, 5 (2), 15. https://doi.org/10.3390/biologics5020015
- Ju, H. J., Kim, J. Y., Jeong, D. H., Lee, M.-S., Kim, G. M., Bae, J. M., Lee, J. H. (2025). Additional Use of Hyaluronic Acid-Based Dissolving Microneedle Patches to Treat Psoriatic Plaques: A Randomized Controlled Trial. Annals of Dermatology, 37 (2), 105. https://doi.org/10.5021/ad.24.024
- Babakurd, F. M., Azzawi, S. K., Alkhouli, M., Al-Nerabieah, Z. (2024). Evaluation of EMLA cream with microneedle patches in palatal anesthesia in children: a randomized controlled clinical trial. Scientific Reports, 14 (1). https://doi.org/10.1038/s41598-024-66212-9
- Ding, Y., Wang, J., Li, J., Cheng, Y., Zhou, S., Zhang, Y. et al. (2025). Tβ4‐Engineered ADSC Extracellular Vesicles Rescue Cell Senescence Through Separable Microneedle Patches for Diabetic Wound Healing. Advanced Science, 12 (26). https://doi.org/10.1002/advs.202505009
- Zheng, K., Zhou, T., Xiao, E., Wei, Q., Zhao, C. (2023). Human collagen decorating microneedle patches for transdermal therapy. Journal of Polymer Science, 62 (14), 3171–3182. https://doi.org/10.1002/pol.20230597
- La Malfa, F., van Hulst, I., Maaden, K., Ossendorp, F., Staufer, U. (2023). Evaluation of microneedle patches for improved intradermal delivery of molecularly-defined cancer vaccines. ResearchGate. https://doi.org/10.13140/RG.2.2.21124.50560
- Lee, M., Jeong, D., Yoon, K., Jin, J., Back, Y. W., Jang, I.-T. et al. (2025). Inactivated mycobacterium paragordonae delivered via microneedle patches as a novel tuberculosis booster vaccine. Human Vaccines & Immunotherapeutics, 21 (1). https://doi.org/10.1080/21645515.2025.2507473
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Liubov Bodnar, Tetiana Kovalova, Natalia Sydora, Oleksandr Shmalko, Ihor Berdey, Liliia Vyshnevska

This work is licensed under a Creative Commons Attribution 4.0 International License.
Our journal abides by the Creative Commons Attribution 4.0 International License copyright rights and permissions for open access journals.
Authors, who are published in this journal, agree to the following conditions:
1. The authors reserve the right to authorship of the work and pass the first publication right of this work to the journal under the terms of a Creative Commons Attribution 4.0 International License, which allows others to freely distribute the published research with the obligatory reference to the authors of the original work and the first publication of the work in this journal.
2. The authors have the right to conclude separate supplement agreements that relate to non-exclusive work distribution in the form in which it has been published by the journal (for example, to upload the work to the online storage of the journal or publish it as part of a monograph), provided that the reference to the first publication of the work in this journal is included.
3. Authors have the right to store the final accepted version of the article in an institutional, thematic, or any other repository to ensure visibility and accessibility.






